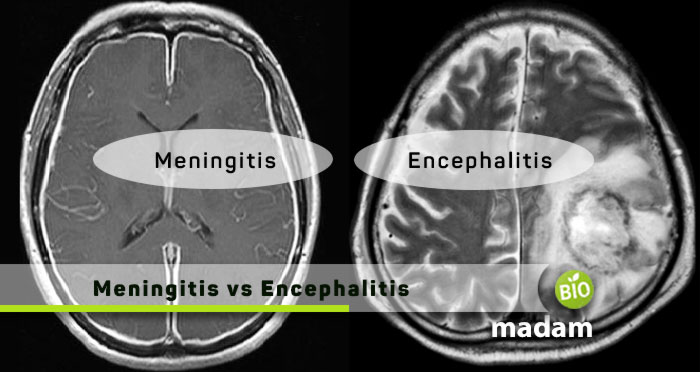
Meningitis and encephalitis are similar terms that refers to the inflammation in the brain. However, when specifically studying, these terms refer to inflammation in certain spaces. Meningitis is the inflammation in the meninges; the membranes that surround the brain, while encephalitis is the inflammation of the brain itself. They occur when any external antigen or pathogen might have entered the brain, leading to infections.
Keep reading to learn all the differences between meningitis and encephalitis.
Comparison Table
| Characteristics | Meningitis | Encephalitis |
| Definition | Inflammation of meninges | Inflammation of brain parenchyma |
| Affected Organs | Brain & spinal cord | Brain |
| Symptoms | Neck stiffness and photophobia | Lethargy and personality disorders |
| Pathogens | S, pneumonia, Hib, L. monocytogenes, and Neisseria meningitidis | Poliovirus, HSV-1, VZV, mycoplasma, and anopheles |
| Vectors | Saliva, stool, or fluid contact | Mosquitoes and mammals |
| Treatment | Antibiotics and antifungals | Antivirals |
| Precautions | Wear masks and gloves | Apply mosquito repellent |
| Seizures | Rare | Common |
What is Meningitis?
Meningitis is the inflammation of the meninges, which is the membrane surrounding the brain and spinal cord. The inflammation causes massive destruction in the cranium, such as swelling, and then puts pressure on the brain; as a result, intracranial pressure increases.
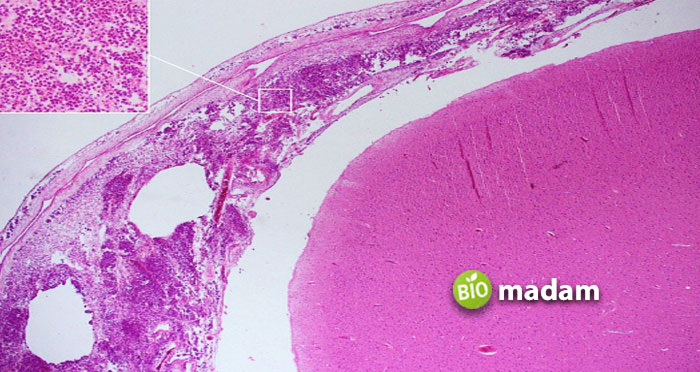
Symptoms of Meningitis
Patients will likely show a combination of signs and symptoms that include:
- Fever
- Severe headache
- Nausea or vomiting
- Photosensitivity
- Nuchal rigidity (neck stiffness)
Patients may also experience altered mental states such as drowsiness, delirium, and confusion. If left untreated, it may spread to the brain tissues resulting in loss of sensory and motor neural functions, coma, or even death.
In addition, healthcare workers may also seek out two specific signs of the infection:
Kernig’s Sign: Let the Patient lie down horizontally. Start raising one leg slowly, then gradually straighten their leg at 900. Severe pain in the back or thigh on moving further can be a sign of meningitis.
Brudzinski’s Sign: First, the person lies horizontally. The doctor carefully grips the head from behind and positions the other hand on the chest. Passively flex the neck forward. Examine the movements of the knees and hips. The person experiences pain and flexes the knees in meningitis.
Causes of Meningitis
Meningitis is caused primarily by viruses and bacteria. Viruses are the common cause, whereas bacteria are rare, however, bacteria are the most contagious source that leads to life-threatening diseases or conditions. Non-infectious causes include some autoimmune disorders, head injuries, and certain medications. Bacterial meningitis transmits through saliva, nasal discharge, feces, or respiratory secretions (usually via coughing). Children who do not receive routine vaccinations are more prone to develop the disease.
Diagnosis of Meningitis
Lumbar Puncture Test: It helps examine cerebrospinal fluid by inserting a needle in the lower back to remove CSF. The lumbar puncture test detects whether it is a bacterial or viral infection.
Laboratory Tests:
- Blood
- Urine
- MRI and CT Scans
Treatment of Meningitis
Bacterial meningitis treatment includes initiating empiric antibiotic therapy, followed by direct antibiotic therapy after microbial identification. Doctors recommend steroid therapy to reduce inflammation. Further close monitoring of the individuals for neurological complications is required. Viral meningitis gets better with antiviral drugs.
What is Encephalitis?
Encephalitis is a condition in which inflammation occurs in the brain parenchyma. It is not very common, but can be life-threatening. Anyone can have encephalitis. However, very old or very young people are at a higher risk of infection.
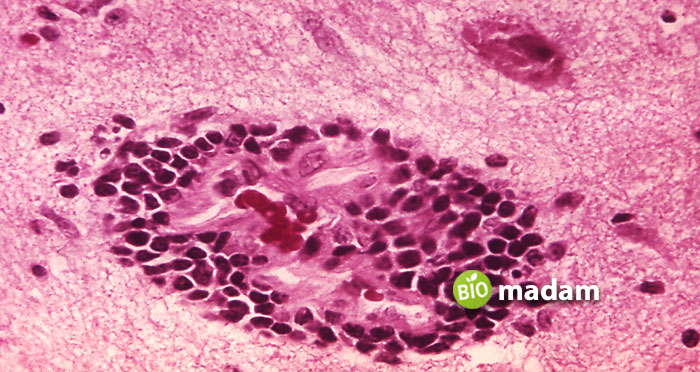
Symptoms of Encephalitis
Symptoms of encephalitis commonly include:
- Fever symptoms
- Depression
- Confusion
- Lethargy
- Hallucination
- Agitation
- Behavior disorders
- Personality changes
- Psychotic states
- Ataxia (difficulty walking)
- Difficulty speaking
- Involuntary muscle movement
Causes of Encephalitis
Encephalitis may be caused by different viruses and bacteria including rabies, enteroviruses, mosquito-borne viruses, herpes viruses, tick-borne viruses, and childhood infections.
Diagnosis of Encephalitis
Encephalitis tests may include the following:
- MRI or CT scans of the brain
- Lumbar puncture test
- EEG
- Blood test
- Urine sampling
- Stool tests
- Sputum culture
- Biopsy of affected brain tissue
- Intracranial pressure monitoring (ICP)
Treatment for Encephalitis
Early detection and effective treatment of the underlying cause are essential. People may need antiviral drugs to treat viral infections of the brain. Antibiotics treat the underlying bacterial infection. Immunotherapy, such as steroids, intravenous antibodies, or plasmapheresis, may help with autoimmune encephalitis. Moreover, medicines like analgesics for high temperatures, antibiotics to clear infection, and other drugs that manage epileptic fits are given.
Vaccines for measles, mumps, rubella, and chickenpox can decrease the number of cases of viral encephalitis. Herpes simplex virus types 1 and 2, varicella-zoster virus, and enteroviruses are viruses causing the infection. Mosquitoes, ticks, and other parasites can also transmit viral encephalitis. People who already have HIV/AIDS, use immuno-suppressive medications, and are immune-compromised are more likely to develop encephalitis.
Difference Between Meningitis and Encephalitis
Definition
Meningitis
It is the inflammation of the protective layer of the brain and spinal cord.
Encephalitis
On the contrary, encephalitis is the inflammation of brain tissues (parenchyma).
Symptoms
Meningitis
Meningitis shows hallmark symptoms of stiffness in the neck and photophobia.
Encephalitis
Patients have behavior changes, personality disorders, and lethargy in encephalitis.
Pathogens
Meningitis
Streptococcus pneumonia causes certain disease and meningeal infection in infants, children, and adults. Besides, Neisseria meningitidis, Listeria monocytogenes, and the virus (Haemophilus influenzae) are the common pathogens causing meningitis.
Encephalitis
Common viruses causing encephalitis include the poliovirus, herpes simplex virus-1, varicella zoster, and some bacteria like mycoplasma, and malaria.
Treatment
Meningitis
Therapy depends on the pathogen, but the patient first receives empirical antibiotic therapy like ampicillin. For fungal meningitis, amphotericin B is the initial treatment.
Encephalitis
Alternatively, patients generally receive acyclovir medication for herpes simplex and varicella zoster pathogens.
Precautions
Meningitis
Healthcare workers should wear masks and gloves and take necessary measures when contacting patients.
Encephalitis
On the other hand, use insect and mosquito repellent to avoid encephalitis spread via mosquitoes and tickles.
Vectors
Meningitis
An infected person can spread the disease via saliva, stool, or fluid contact.
Encephalitis
While encephalitis can spread through mosquitoes and mammals.
Seizures
Meningitis
Seizures are uncommon or may be minimal.
Encephalitis
Whereas, convulsions or seizures can become more common.
The Bottom Line
Meningitis and encephalitis refers to inflammation in the brain and spinal cord. The major difference between meningitis and encephalitis is that meningitis may affect the brain as well as the spinal cord. On the other hand, encephalitis is the infection of the brain parenchyma. They are typically caused by bacteria and viruses. They are uncommon, yet may spread through different vectors. Depending on the causative agent, your doctor may prescribe antivirals, antibiotics, or even vaccines to treat the infection.
FAQs
What is worse meningitis or encephalitis?
As they both affect the nervous system, there is no evidence about which one is more serious. They must be treated in time or they may cause severe damage to sensory and motor function.
Can you have encephalitis and meningitis?
Yes, it is possible to have both meningitis and encephalitis at the same time, known as meningoencephalitis. It usually happens when the membranes also get inflamed following the inflammation in the brain.
What is meningitis commonly mistaken for?
The symptoms of meningitis are typically similar to flu symptoms, leading to an improper diagnosis. It is critical to diagnose the condition properly to follow an adequate treatment regimen.

The Biomadam Content Team develops and manages educational and informational articles published on Biomadam. Content is prepared using standard reference materials and follows internal editorial guidelines to ensure clarity and consistency.