The anatomy and physiology of the human body comprise bones, muscles, tendons, and ligaments. Bones are dynamic, changing in response to the stresses and strains placed upon them. The most numerous type of cells found in bone tissue, osteocytes, are responsible for this extraordinary versatility. Bone cells rely on osteocytes’ complex web-like network for communication, which plays a vital role in bone creation, maintenance, and repair.
Let’s tell you more about the functions of osteocytes in bones to see how these cells work to maintain a robust and healthy skeleton.
What are Osteocytes?
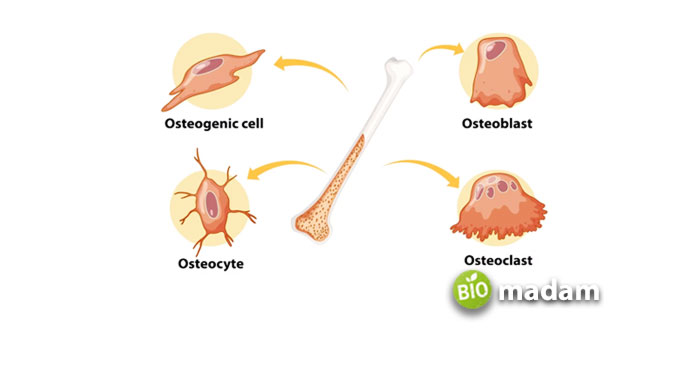
The word “osteo” relates to bones, and osteoclasts, osteoblasts, and osteocytes are the three types of cells in bones. Osteocytes are mature bone cells present within the mineralized matrix of bone tissue. Osteocytes develop from osteoblasts and affix to the bone matrix. A fully developed human being has roughly 42 billion osteocytes.
Functions of Osteocytes
There is obviously a certain role for osteocytes, being very abundant in the body. We will look into these, one by one:
Mechanical Support
Osteocytes help to provide mechanical support to the bone tissue by secreting and maintaining the mineralized matrix that makes up the structure of bone. Through canaliculi, tiny channels embedded within the mineralized bone, tissue communicates with neighboring cells. This network allows them to detect and respond to mechanical stresses and strains on the bone. Thus enabling them to help regulate bone growth and remodeling.
In a basic multicellular unit (BMU), osteocytes regulate the activity of osteoblasts and osteoclasts. Osteocytes produce an inhibitory signal transmitted through their cell processes to osteoblasts in order to attract osteoblasts and promote bone formation.
Regulation of Bone Remodelling
Osteocytes are also involved in regulating bone remodeling, the process by which bone tissue is continually broken down and rebuilt throughout life. They play a crucial role in controlling bone tissue production.
Upon bone fracture, osteocytes with glutamate transporters inside of them produce nerve growth factors, suggesting the presence of a sensing and information transfer system. The loss of osteocytes in the bone leads to an increase in bone resorption and a decrease in bone formation. It may also result in the loss of trabecular bone and a failure to respond to unloading in an experimental model.
Control of Calcium and Phosphate Metabolism
Osteocytes play a crucial role as an endocrine regulator to metabolize minerals. They can sense changes in the levels of these minerals in the blood and respond by releasing or absorbing them from the surrounding bone tissue. They maintain the delicate balance of these minerals in the body, which is crucial for various physiological processes.
Sclerostin, other osteocyte-specific proteins, and molecules that control phosphate and biomineralization, such as PHEX, DMP-1, MEPE, and FGF-23, play a role in mineral metabolism.
Prevention from Bone-Related Diseases
Research shows that there may be a connection between osteocyte regulation and disease prevention. Lynda Bonewald discovered that osteocytes produce FGF23, which circulates in the blood and stimulates the kidneys to excrete phosphorus.
Communication with Other Bone Cells
Osteocytes can communicate with other bone cells through the network of canaliculi that connects them. They can signal to other bone cells to stimulate or inhibit bone remodeling and help repair damaged bone tissue.
Structure of Osteocytes
Osteocytes are stellate, measuring 7 micrometers deep and 15 micrometers long. The structure of osteocyte constitutes the following:
Cell Body
The central part of the osteocyte is its cell body, which is star-shaped. Cell body diameters range from 5-20 micrometers, with each cell sporting 40-60 processes; intercellular distances average 20-30 micrometers.
Cell Processes
Osteocytes have several long and slender cell processes that extend from the cell body into the canaliculi. These processes communicate with other osteocytes and exchange nutrients and waste products.
Nucleus
Osteocytes have a large, centrally located cell nucleus containing the genetic material necessary for cell function. The nucleus is membrane-bound and oriented towards the vascular side.
Organelles
The cell body of osteocytes contains all the usual organelles found in eukaryotic cells, including mitochondria, Golgi apparatus, endoplasmic reticulum, and lysosomes.
Lacunae
Osteocytes reside within small cavities in the bone matrix called lacunae. Each lacuna contains one osteocyte.
Canaliculi
Osteocytes connect to the bone surface by tiny canaliculi channels. These channels allow the communication and exchange of nutrients and waste products between osteocytes and the bone surface.
The Bottom Line
Osteocytes are the longest bone cells in the body making up 90% – 95% of cells in bones. They are formed from osteoblasts that are buried in the mineral matrix of bones. They contribute to the regulation of local mineral deposition in the bone matrix. They act as endocrine cells producing factors that target distant tissues and organs to regulate phosphate transport. Osteocytes also have a role in mechanical support, communication with other bone cells, and prevention of bone-related diseases.
FAQs
What are the functions of osteoclasts?
Osteoclasts are also bone cells. They are involved in the degradation of the bone to remodel it and mediate the loss of bone in pathological conditions. They develop from monocyte/myeloid regions in the blood.
What is the function of osteocytes in lacunae?
Osteocytes contribute to the homeostatic adaptation of bone to mechanical forces within the lacunae. They promote bone repair and maintain bone mass even when they are dying.
What is the function of osteoblasts?
Osteoblasts are involved in laying down new bones during skeletal redevelopment and remodeling. They interact with other types of cells within the bones, such as the hematopoietic stem cells.
Do osteoclasts destroy osteocytes?
Research has shown that osteoclasts engulfed a few osteocytes during a study when released from osteocytic lacunae during bone remodeling.
How do osteocytes remove waste?
Osteocytes receive nutrients and oxygen and remove wastes and carbon dioxide by diffusion through the extended processes in the canaliculi.
Do osteoclasts remove calcium?
Osteoclasts produce acid phosphatase, among other enzymes, that dissolve phosphorus, calcium, and organic collagen in the bone.
What activates osteoclasts?
PTH and Vitamin D increase the activity of osteoclasts, stimulating bone reabsorption, and leading to increased blood calcium levels.

The Biomadam Content Team develops and manages educational and informational articles published on Biomadam. Content is prepared using standard reference materials and follows internal editorial guidelines to ensure clarity and consistency.